For payers, Eviti Connect streamlines the authorization of oncology treatment, ensuring prescription of high-quality, high-value care and setting patients on the path to appropriate treatment sooner. Powered by the renowned Eviti Evidence-based Medical Library, Eviti Connect minimizes payer risk while simultaneously placing evidence-based treatments in the hands of providers.
Minimize Risk. Maximize Care.
Eliminate unwarranted variability in care through the application of nationally-accepted treatment standards at the moment of clinical prescription. The automated process reduces the administrative burdens of obtaining and providing authorizations and ensures appropriate reimbursement at the regimen level, aligning payers and physicians in the best interests of patients while limiting appeals and denials.
When a physician-recommended oncology treatment plan isn’t automatically approved, it enters a rigorous clinical review process to determine that the proposed treatment regimen is the best fit for a particular patient.
Cancer drug costs are expected to double in the next two years.
Selecting an evidence-based treatment that offers the best possible outcome at a lower cost than a competing therapy creates value for payers, providers, and patients alike.
Value-Based Care: A Win for Everyone
Meeting the needs of payers, providers, and patients is complex, but it’s not impossible. Eviti Connect clears the way for value-based oncology care that benefits everyone involved.
- Patients have peace of mind that they are receiving the best treatment for their disease.
- Physicians can prescribe evidence-based care and receive appropriate reimbursement from the payer—with near real-time communications with the payer.
- Payers are assured the member is getting the right care at the best cost.
Empowering Better Oncology Decisions
Enable high-quality oncology care
Provide oncologists in your network with access to a comprehensive library of evidence-based treatment options which can be filtered and pinpointed to the patient’s specific diagnosis for optimal decision making.
Streamline operational workflows
Improve claim processing efficiency and reduce denials and appeals with an Eviti code. This code is provided when a physician chooses an evidence-based regimen, thereby validating appropriate treatment and pre-adjudicating the claim.
Integrate medical policies
Automate the process of verifying that treatments meet your plan’s medical policy and plan language before the treatment is selected and ordered.
Ensure appropriate reimbursement
Have visibility at the moment of prescribing, while your network providers are assured the treatments they recommend meet the clinical requirements for reimbursement.
Indicate payer preferences
Highlight preferred regimens to indicate treatments aligned with payer-specific observed outcomes or higher reimbursement opportunities.
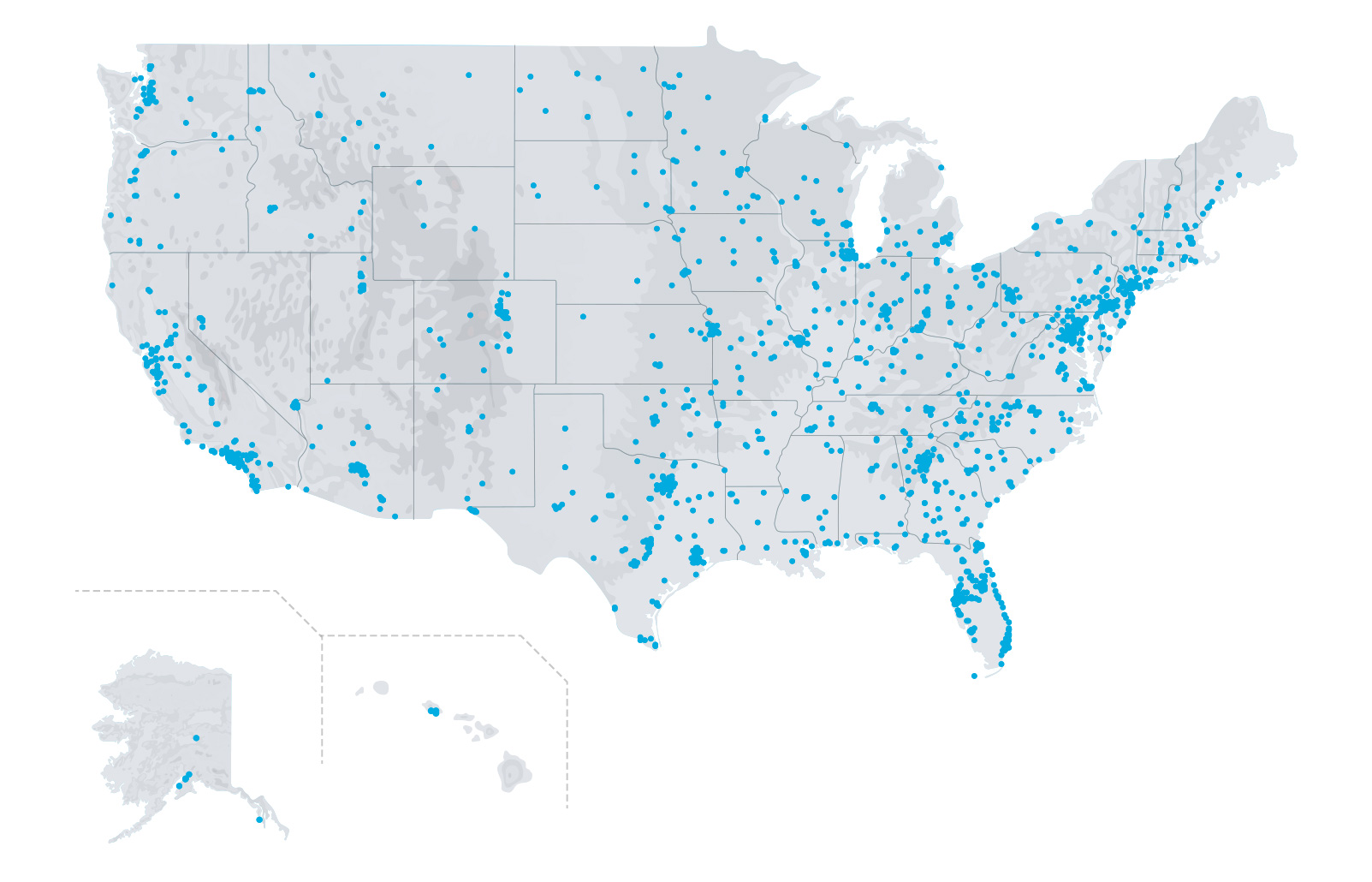
Provider Adoption
Eviti Connect is used by over 7,700 practices nationwide.